Relationship Between Socioeconomic Status by Place of Residence and Body Mass Index in Patients With Type 1 Diabetes Mellitus Attended at a Specialized Pediatric Institute in Lima, Peru
DOI:
https://doi.org/10.58597/rpe.v4i1.93Keywords:
Type 1 Diabetes Mellitus, Body Mass Index, Overweight, Obesity, Underweight, Socioeconomic Status, Poverty, Children, AdolescentsAbstract
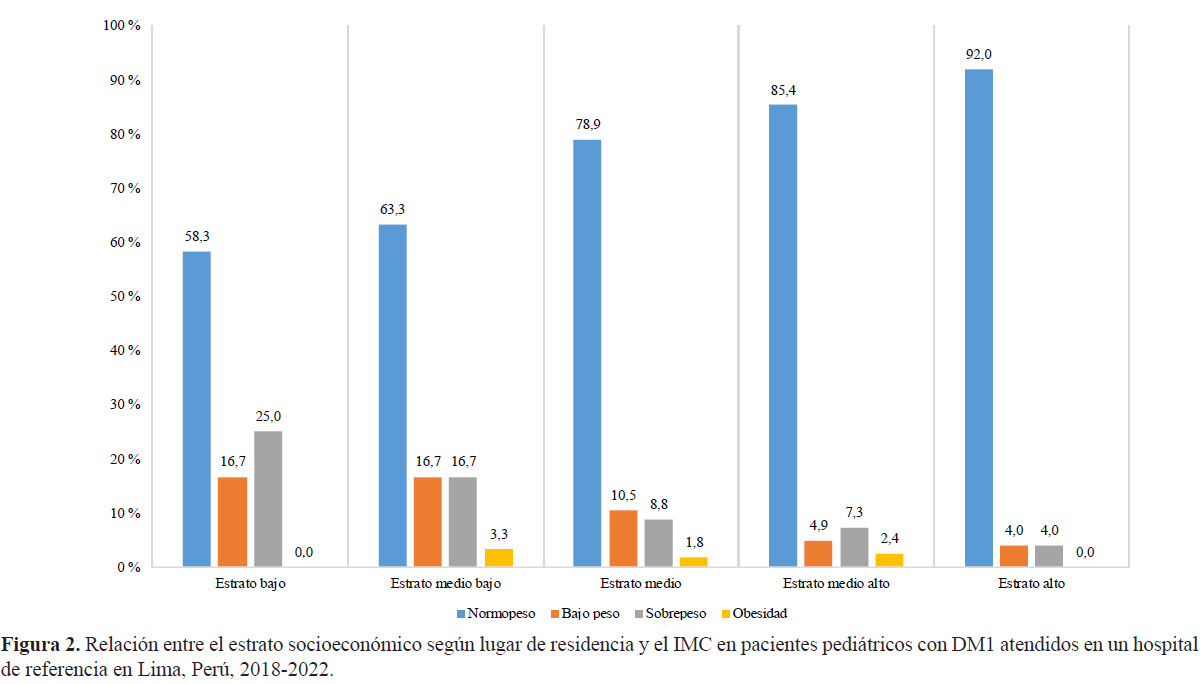
Objective: To explore the relationship between socioeconomic status, based on place of residence, and body mass index (BMI) in patients with type 1 diabetes mellitus (T1DM) treated at a specialized pediatric institute in Lima, Peru. Materials and Methods: An observational, analytical, and cross-sectional study was conducted through a review of medical records of patients aged 1 to 18 years diagnosed with T1DM, residing in Metropolitan Lima and Callao, and treated at an endocrinology outpatient clinic between 2018 and 2022. Socioeconomic status was categorized as low (low and lower-middle) and middle-high (middle, upper-middle, and high). BMI was classified as healthy or unhealthy weight. To evaluate the association, generalized linear models from the Poisson family with robust variance were used to calculate the prevalence ratio (PR) and 95% confidence intervals (CI), considering a p-value <0.05 as statistically significant. Results: A total of 165 patients with T1DM were included, with a mean age of 9.90 ± 4.06 years, and 50.9% were male. A significant association was found between BMI and socioeconomic status (p=0.013). Additionally, belonging to a low socioeconomic stratum was associated with a higher prevalence of unhealthy weight (PR: 2.39; 95% CI: 1.39-4.11, p=0.002). Conclusion: Patients with T1DM from lower socioeconomic strata based on place of residence have a higher prevalence of unhealthy weight compared to those from middle and high strata. These findings suggest that socioeconomic factors may influence the nutritional status of this population, highlighting the need for targeted intervention strategies.
Downloads
References
Rodger W, Joseph’s Health Centre S, St G. Insulin-dependent (type I) diabetes mellitus. CMAJ. 1991;145(10):1227. Disponible en: https://pmc.ncbi.nlm.nih.gov/articles/PMC1335936/pdf/cmaj00251-0045.pdf
International Diabetes Federation. IDF Diabetes Atlas 10th edition; Disponible en: www.diabetesatlas.org
Yau M, Maclaren NK, Sperling MA. Etiology and Pathogenesis of Diabetes Mellitus in Children and Adolescents. [Internet]. South Dartmouth (MA): MDText.com, Inc.; 2000-2025. Disponible en: https://www.ncbi.nlm.nih.gov/books/NBK498653/
Mayer-Davis EJ, Kahkoska AR, Jefferies C, Dabelea D, Balde N, Gong CX, et al. ISPAD Clinical Practice Consensus Guidelines 2018: Definition, epidemiology, and classification of diabetes in children and adolescents. Pediatr Diabetes. 2018;19(Suppl 27):7-19. doi: 10.1111/pedi.12773.
Díez-Fernández A, Ruiz-Grao MC, Mesas AE, Martinez-Vizcaino V, Garrido-Miguel M. Type 1 diabetes incidence trends in children and adolescents aged 0-14 years in Europe: a systematic review and meta-analysis protocol. BMJ Open[Internet]. 2021;11(10):e054962. doi: 10.1136/bmjopen-2021-054962.
Villena JE. Epidemiología de la Diabetes Mellitus en el Perú. Diagnóstico [Internet]. 2019;55(4):173–81. Disponible en: https://revistadiagnostico.fihu.org.pe/index.php/diagnostico/article/view/21/47
Gomber A, Ward ZJ, Ross C, Owais M, Mita C, Yeh JM, et al. Variation in the incidence of type 1 diabetes mellitus in children and adolescents by world region and country income group: A scoping review. PLOS Glob Public Health. 2022;2(11):e0001099. doi: 10.1371/journal.pgph.0001099. Erratum in: PLOS Glob Public Health. 2024;4(6):e0003398. doi: 10.1371/journal.pgph.0003398.
Siddiqui F, Salam RA, Lassi ZS, Das JK. The Intertwined Relationship Between Malnutrition and Poverty. Front Public Health. 2020; 8:453. doi: 10.3389/fpubh.2020.00453.
Centers for Disease Control and Prevention. About Body Mass Index for Children and Adolescents [Internet]. Atlanta: CDC; [citado el 04 de diciembre de 2024]. Disponible en: https://www.cdc.gov/bmi/faq/index.html
Cunha MPL, Marques RC, Dórea JG. Child Nutritional Status in the Changing Socioeconomic Region of the Northern Amazon, Brazil. Int J Environ Res Public Health. 2017; 15(1):15. doi: 10.3390/ijerph15010015.
Cordeiro LS, Otis NP, Sibeko L, Nelson-Peterman J. Rural-urban disparities in the nutritional status of younger adolescents in Tanzania. PLoS One. 2021; 16(12):e0261480. doi: 10.1371/journal.pone.0261480.
Tigga PL, Sen J, Mondal N. Association of Some Socio-Economic and Socio-Demographic Variables with Wasting Among Pre-School Children of North Bengal, India. Ethiop J Health Sci. 2015; 25(1): 63-72. doi: 10.4314/ejhs.v25i1.9.
Liese AD, Puett RC, Lamichhane AP, Nichols MD, Dabelea D, Lawson AB, et al. Neighborhood level risk factors for type 1 diabetes in youth: the SEARCH case-control study. Int J Health Geogr. 2012;11:1. doi: 10.1186/1476-072X-11-1.
Kivimäki M, Vahtera J, Tabák AG, Halonen JI, Vineis P, Pentti J, et al. Neighbourhood socioeconomic disadvantage, risk factors, and diabetes from childhood to middle age in the Young Finns Study: a cohort study. Lancet Public Health. 2018;3(8):e365-e373. doi: 10.1016/S2468-2667(18)30111-7. Epub 2018 Jul 18. Erratum in: Lancet Public Health. 2018;3(11):e522. doi: 10.1016/S2468-2667(18)30215-9.
Zhou S, Raat H, You Y, Santos S, van Grieken A, Wang H, et al. Change in neighborhood socioeconomic status and childhood weight status and body composition from birth to adolescence. Int J Obes (Lond). 2024;48(5):646-653. doi: 10.1038/s41366-023-01454-7.
Instituto Nacional de Estadística e Informática. Evolución de la Pobreza Monetaria 2009-2020 [Internet]. 2021[citado el 06 de diciembre de 2024]. Disponible en: https://cdn.www.gob.pe/uploads/document/file/3288764/Informe%20T%C3%A9cnico.pdf
Instituto Nacional de Estadística e Informática [Internet] [citado el 06 de diciembre de 2024]. Disponible en: https://m.inei.gob.pe/prensa/noticias/pobreza-monetaria-afecto-al-275-de-la-poblacion-del-pais-en-el-ano-2022-14391/
Instituto Nacional de Estadística e Informática. Metodología para la medición de la pobreza monetaria [Internet]. Lima: INEI; 2017 [citado el 07 de diciembre de 2024]. Disponible en: https://www.inei.gob.pe/media/cifras_de_pobreza/nota01.pdf
Instituto Nacional de Salud del Niño. Información Institucional [Internet] [citado el 07 de diciembre de 2024]. Lima: INSN; 2024. Disponible en: http://www.insn.gob.pe/institucional/mision-vision
Gomes MB, Conte D, Drummond KRG, Mallmann F, Pinheiro AA, Leal FSL, et al. Overweight/obesity in adolescents with type 1 diabetes belonging to an admixed population. A Brazilian multicenter study. Diabetol Metab Syndr. 2022; 14(1):1. doi: 10.1186/s13098-021-00759-9.
Da Costa VM, de Carvalho Padilha P, de Lima GC, Ferreira AA, Luescher JL, Porto L, et al. Overweight among children and adolescent with type I diabetes mellitus: prevalence and associated factors. Diabetol Metab Syndr. 2016; 8:39. doi: 10.1186/s13098-016-0154-4.
Pastor-Fajardo MT, Fajardo-Giménez MT, Bosch-Giménez VM, Pastor-Rosado J. Changes from 1986 to 2018 in the prevalence of obesity and overweight, metabolic control and treatment in children with type 1 diabetes mellitus in a Mediterranean area of Southeast Spain. BMC Pediatr. 2022;22(1):274. doi: 10.1186/s12887-022-03330-1.
Mühlhauser I, Overmann H, Bender R, Bott U, Jörgens V, Trautner C, et al. Social status and the quality of care for adult people with type I (insulin-dependent) diabetes mellitus--a population-based study. Diabetologia. 1998;41(10):1139–50. Disponible en: https://pubmed.ncbi.nlm.nih.gov/9794099/
Hussein SA, Ibrahim BA, Abdullah WH. Nutritional status of children and adolescents with Type 1 Diabetes Mellitus in Baghdad: a case-control study. J Med Life. 2023;16(2):254-260. doi: 10.25122/jml-2022-0233.
Mönkemöller K, Müller-Godeffroy E, Lilienthal E, Heidtmann B, Becker M, Feldhahn L, et al. The association between socio-economic status and diabetes care and outcome in children with diabetes type 1 in Germany: The DIAS study (diabetes and social disparities). Pediatr Diabetes. 2019;20(5):637-644. doi: 10.1111/pedi.12847.
Deladoëy J, Henderson M, Geoffroy L. Linear association between household income and metabolic control in children with insulin-dependent diabetes mellitus despite free access to health care. J Clin Endocrinol Metab. 2013;98(5): E882-5. doi: 10.1210/jc.2013-1212.
Lalanne-Mistrih ML, Bonhoure A, Messier V, Boudreau V, Lebbar M, Talbo MK, et al. Overweight and Obesity in People Living with Type 1 Diabetes: A Cross-Sectional Analysis of the BETTER Registry. Diabetes Metab Res Rev. 2024;40(6): e3837. doi: 10.1002/dmrr.3837.
Davison KA, Negrato CA, Cobas R, Matheus A, Tannus L, Palma CS et al. Brazilian Type 1 Diabetes Study Group (BrazDiab1SG). Relationship between adherence to diet, glycemic control and cardiovascular risk factors in patients with type 1 diabetes: a nationwide survey in Brazil. Nutr J.2014; 13:19. doi: 10.1186/1475-2891-13-19
Chaparro MP, Lopez MA, Hernandez J, Brewer JD, Santos MP, Paz-Soldan VA. The association between the observed and perceived neighbourhood food environment and household food insecurity in a low-income district in Lima, Peru. J Nutr Sci. 2022;11: e86. doi: 10.1017/jns.2022.88.
Morales-Cahuancama B, Dolores-Maldonado G, Hinojosa-Mamani P, Bautista-Olortegui W, Quispe-Gala C, Huamán-Espino L, et al. Analysis of the distribution of macronutrients of food baskets delivered by municipalities during the COVID-19 pandemic in Peru. Rev Peru Med Exp Salud Publica. 2022;39(1):6-14. doi: 10.17843/rpmesp.2022.391.9742.
Vilar-Compte M, Burrola-Méndez S, Lozano-Marrufo A, Ferré-Eguiluz I, Flores D, Gaitán-Rossi P, et al. Urban poverty and nutrition challenges associated with accessibility to a healthy diet: a global systematic literature review. Int J Equity Health. 2021;20(1):40. doi: 10.1186/s12939-020-01330-0.
Morgenstern M, Sargent JD, Hanewinkel R. Relation between socioeconomic status and body mass index: evidence of an indirect path via television use. Arch Pediatr Adolesc Med. 2009;163(8):731-8. doi: 10.1001/archpediatrics.2009.78.
Carroll-Scott A, Gilstad-Hayden K, Rosenthal L, Eldahan A, McCaslin C, Peters SM, et al. Associations of Neighborhood and School Socioeconomic and Social Contexts with Body Mass Index Among Urban Preadolescent Students. Am J Public Health. 2015;105(12):2496-502. doi: 10.2105/AJPH.2015.302882.
Ricci-Cabello I, Ruiz-Pérez I, De Labry-Lima AO, Márquez-Calderón S. Do social inequalities exist in terms of the prevention, diagnosis, treatment, control and monitoring of diabetes? A systematic review. Health Soc Care Community. 2010;18(6):572–87. doi: 10.1111/j.1365-2524.2010.00960.x.
Grintsova O, Maier W, Mielck A. Inequalities in health care among patients with type 2 diabetes by individual socio-economic status (SES) and regional deprivation: a systematic literature review. Int J Equity Health. 2014;13(1):43. doi: 10.1186/1475-9276-13-43.
Chaturvedi N, Stephenson JM, Fuller JH. The Relationship Between Socioeconomic Status and Diabetes Control and Complications in the EURODIAB IDDM Complications Study. Diabetes Care. 1996;19(5):423–30. doi:10.2337/diacare.19.5.423
Zgibor JC, Songer TJ, Kelsey SF, Weissfeld J, Drash AL, Becker D, et al. The association of diabetes specialist care with health care practices and glycemic control in patients with type 1 diabetes: a cross-sectional analysis from the Pittsburgh epidemiology of diabetes complications study. Diabetes Care. 2000;23(4):472–6. doi:10.2337/diacare.23.4.472
Downloads
Additional Files
Published
Issue
Section
License
Copyright (c) 2025 Katherine Alexandra Macedo-Hidalgo, Gabriela Julia Huamán-Varillas, Isabel Angélica Pinedo-Torres

This work is licensed under a Creative Commons Attribution 4.0 International License.